Detecting & Diagnosing Eye Diseases
An eye exam is an important part of preventive healthcare. During an eye exam, your optometrist checks your vision quality, and they’ll also check for the development of eye diseases.
Many eye diseases can damage your vision permanently and progress without any noticeable symptoms, particularly in the beginning.
Early identification is crucial for treating and managing eye diseases. If your optometrist catches them early enough, they may be able to slow down progression or prevent vision loss.
Your sight is precious. Safeguard it today with a comprehensive eye exam.
Book AppointmentCONJUNCTIVITIS
Conjunctivitis can be either an irritation or an infection of the membrane that covers the white of the eye and the inside lining of the eyelid. It has become commonly known as “pink eye” due to the significant blood vessel inflammation that can occur.
Allergies and other irritants like air pollution, eye make up, and contact lenses cause irritation conjunctivitis. Infection conjunctivitis has two categories—viral and bacterial. The viral type usually accompanies a cold, fever, sore throat, or flu and is characterized by eye redness and a watery discharge. The bacterial type presents with eye redness, a mucous like discharge, and is usually caused by a staph or strep bacteria.
Some bacterial and viral pinkeye can easily be passed between people, and it is common for children to experience this type of the disease. The symptoms are generally mild and do not pose a serious threat to eye health, but symptoms in newborns should be addressed by a doctor right away to help ensure no vision loss occurs.
Conjunctivitis is treated differently depending on the cause. Most cases can be successfully treated with antibiotics, eye drops, or ointments.
Our Doctors are trained and equipped to make the correct diagnosis of the type of conjunctivitis. In some cases, conjunctivitis can progress to more serious eye condition and vision damage so professional evaluation is important.
ALLERGIES
Because eye allergies are very common, Our Doctors would like to share with you some background information regarding eye allergies.
An allergy is an overreaction by the immune system by normally harmless subjects called allergens. Most people will suffer from at least one allergic reaction at some point in their life.
The most common allergens are pollen, dust mites, pet dander, insect venom and food. When a person encounters an allergen for the first time the immune system mistakenly believes the allergen is a threat and responds by producing anti-bodies to fight them.
These allergic reactions occur because the body produces white blood cells, which bind together to create mast cells. When the body is re-exposed to the same allergen, the mast cell releases chemicals to fight the allergen and protect the body. This results in an allergic response, which can range from uncomfortable to dangerous.
Symptoms may include red, watery and itchy eyes, a runny or stuffed nose, sneezing, sinus pressure, a sore throat, coughing, shortness of breath, chest tightening, and in severe cases, an asthma attack.
While there is no cure, there are ways to prevent or relieve allergy symptoms, such as avoiding specific allergens, taking medication, or immunotherapy.
BLEPHARITIS
Blepharitis is a common condition that causes inflammation of the eyelids. It is characterized by redness, swelling, styes, cysts, and flaky crusts at the eyelid margin and along the lash line. Symptoms include scratchy, swollen, tender, and irritated eyes. Blepharitis can be caused by various types of bacteria, and it may be chronic or acute in presentation. People with skin conditions such as rosacea, acne, and eczema are more prone to have flare ups. Poor facial hygiene can also be a contributing factor.
There are various types of this condition. Anterior blepharitis occurs on the outside of the eye. With it, you may see redness, swelling, and possibly crust near the line of the eyelashes. Posterior blepharitis happens nearer the inside of the eyelid where it contacts the eye. The posterior type can be due to problems with the lubricating meibomian glands inside the eyelids.
Treatment options are abundant and include over the counter remedies and prescription eyedrops and ointments. Occasionally, minor eyelid surgery is necessary to remove cysts when topical treatments are unsuccessful. In rare cases, ongoing treatment may be required to keep the eyes comfortable and symptom-free. Eyelid hygiene can help maintain eye comfort and appearance. Routine care includes frequent face washing, cleaning the scalp, eyelid scrubs, and occasionally doing a soak or warm compress.
Our Doctors will diagnose the specific type of blepharitis during an eye exam.
CATARACTS
A cataract is a clouding of the lens inside the eye. The condition can lead to a decrease in vision if clouding develops enough to obstruct your view. Left untreated, it is the most common cause of blindness in the world.
Cataracts are conventionally treated with surgery. Visual loss occurs because opacification of the lens obstructs light from passing through and being focused on to the retina at the back of the eye.
The most common cause of a cataract is biological aging and over exposure to ultraviolet light. Seeing through a cataract is similar to looking through a foggy window. People with cataracts commonly experience difficulty in appreciating colors and changes in contrast, driving, reading, recognizing faces, and coping with glare from bright lights.
While there is no way guaranteed way to avoid a cataract, wearing everyday eyewear and sunglasses that block 100 percent of UVA and UVB rays can slow the onset, as well as decreasing exposure to direct sunlight.
Cataracts do not need to interfere with your lifestyle. If you are concerned you may be suffering from a cataract, call our office today to schedule an eye health evaluation.
If you have questions regarding cataracts, call our office or ask one of Our Doctors at your next appointment. Make sure you are scheduling yearly eye exams to look for potential symptoms and risk factors of cataracts and other threats to your vision.
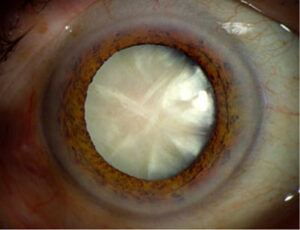
- As we age, the lens in our eye can become cloudy, leading to an impairment of your vision.
- Help to diagnose and manage your cataract.
- If vision is significantly reduced, we can recommend a trusted local surgeon for the operation.
- Perform all the preoperative and postoperative care in our office.
- The proper treatment and management of your cataract can lead to a whole new world of vision, so please do not hesitate to call us to schedule an appointment.
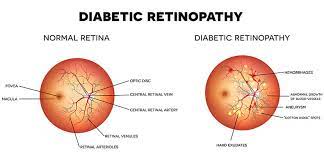
DIABETIC RETINOPATHY
Diabetic retinopathy is damage to the retina caused by complications of diabetes and is the leading cause of blindness in American adults.
It is an ocular manifestation of diabetes, a systemic disease, which affects up to 80 percent of all patients who have had diabetes for 10 years or more. The longer a person has diabetes, the higher his or her chances of developing diabetic retinopathy.
Despite these intimidating statistics, research indicates that at least 90% of new cases could be reduced by preventative monitoring during regular eye examinations and proper treatment.
There are multiple forms of diabetic retinopathy, and only your doctor can determine your particular form. With one form, blood vessels may swell and leak fluid. In another, abnormal new blood vessels grow on the surface of the retina.
In the early stages of diabetic retinopathy, many do not notice a change to their vision because there are little to no symptoms. If an eye doctor does not catch the disease early, one could sustain mild blurriness at near or in the distance, as well as floaters. In severe cases a sudden loss of vision may occur.
Unfortunately, Diabetic Retinopathy can result in permanent damage that cannot be reversed. However, if caught in time, prescribed treatments may slow development and prevent vision loss.
If you have diabetes and are concerned about diabetic retinopathy, schedule an appointment with one of Our Doctors for a comprehensive eye exam and be sure to include it on your patient history form.
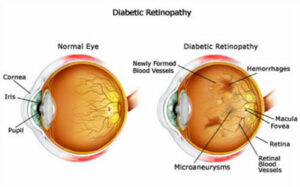
- It is vital that a person diagnosed with diabetes or hypertension has a comprehensive eye exam every year.
- Diabetes can lead to the development of new blood vessels in the back of the eye, which over time may leak and cause damage to the retina, resulting in vision loss.
- Our doctors communicate with your primary care physicians to relay findings, which assist your physician in determining the number and types of medications necessary to maintain proper diabetic control.
- With the aid of advanced digital retinal photography at our office, the earliest changes associated with diabetes are detected.
- In the case of advanced diabetic eye disease, we work closely with board certified retinal specialists in the area to refer patients for sight saving laser treatment and or Avastin injections.
DRY EYE SYNDROME
Dry eye syndrome is a condition in which there are insufficient tears to lubricate and nourish the eye. Tears are necessary for maintaining the health of the front surface of the eye and for providing clear vision. People with dry eyes either do not produce enough tears, or have a poor quality of tears. Dry eye is a common and often chronic problem, particularly in older adults.
With each blink of the eyelids, tears are spread across the front surface of the eye, known as the cornea. Tears provide lubrication, reduce the risk of eye infection, wash away foreign matter in the eye, and keep the surface of the eyes smooth and clear.
Excess tears in the eyes flow into small drainage ducts, in the inner corners of the eyelids, which drain in the back of the nose. Dry eyes can result from an improper balance of tear production and drainage.
People with dry eyes may experience symptoms of irritated, gritty, scratchy, or burning eyes, a feeling of something in their eyes, excess watering, and blurred vision. Advanced dry eyes may damage the front surface of the eye and impair vision.
The development of dry eyes can have many causes including age, gender, medications, medical conditions, environmental conditions and more.
Dry eyes can be a chronic condition, but your eye doctor can prescribe treatment to keep your eyes healthy, more comfortable, and prevent your vision from being affected. Specific treatments aim to restore or maintain the normal amount of tears in the eye to minimize dryness and related discomfort and to maintain eye health. If you believe you are suffering from dry eye syndrome, make an appointment with The Optometry Center today.
GLAUCOMA
Glaucoma is a an eye disease in which damage to the optic nerve leads to progressive, irreversible vision loss. Once thought to be only a high eye pressure problem, it is now known to be a more complex condition. There isn’t one specific level of eye pressure that leads to vision disturbances. Many factors cause this condition and it can only be found with a comprehensive eye exam. Because people rarely experience symptoms, those with increased risk factors are especially encouraged to see an eye doctor regularly for evaluation. People of all ages are at risk for developing glaucoma, so talk to your eye care professional about screening for the condition.
Glaucoma is a complicated disease in which damage to the optic nerve leads to progressive, irreversible vision loss and is the second leading cause of blindness.
The most common form of glaucoma occurs when the eye’s drainage canals become clogged over time. The inner eye pressure, also called intraocular pressure or IOP, rises because the correct amount of fluid can’t drain out of the eye. With the most common form of glaucoma, the entrances to the drainage canals are clear, and should be working correctly. However, the clogging problem occurs further inside the drainage canals (similar to a clogged pipe below the drain of a sink).
Most people will not experience symptoms, nor will they have any early warning signs. If open angle glaucoma is not diagnosed and treated, it can cause a gradual loss of vision. The disease develops slowly and sometimes without visible sight loss for many years. It usually responds well to medication, especially if caught early and treated.
While anyone at any age can develop glaucoma, a higher risk is associated due to family history, individuals over 40 years of age, diabetics, individuals of african or mediterranean descent, as well as those who’ve experienced an eye injury or trauma.
People with glaucoma rarely experience symptoms, but each day, their vision becomes less and less clear. For this reason, routine eye examinations are more important than ever to help identify symptoms. Your eye doctor can detect elevated pressure within the eye, which can cause damage to the optic nerve that carries images to the brain. Left untreated, glaucoma can cause blindness. Call your eye doctor today for more information.
Our Doctors may become suspicious of glaucoma during this exam and order special tests to help in making the diagnosis. From there, the best treatment option will be decided.

- Glaucoma is a problem when the optic nerve inside your eye is damaged from either having too high of a fluid pressure and or having many of the other risk factors involved.
- This is called “the silent thief” as vision is lost slowly through destruction of the nerve fibers comprising the optic nerve, leading to side vision loss.
- If not controlled, this can lead to eventual blindness.
- We screen for glaucoma during our annual comprehensive eye examinations and if a suspicion arises, we will recommend that you return for further in depth glaucoma testing.
- This testing will include extensive peripheral field analysis, 3D optic nerve digital photography, laser light imaging and measurements of the optic nerve as well as eye pressure profiles taken during different times of the day.
- From these and other test results, we will determine whether you are presently diagnosed with glaucoma, a glaucoma suspect, or simply demonstrate glaucoma-like qualities but are completely normal for you.
- Once the diagnosis is made, the doctor will explain your status and recommend the best course of action to fit the diagnosis.
MACULAR DEGENERATION
Age-related macular degeneration, often referred to as AMD, is a medical condition which usually affects older adults. This vision stealing disease is a result of degeneration to the macula, and results in a loss of vision in the center of the visual field because of damage to the retina. It occurs in “dry” and “wet” forms and is a major cause of blindness and visual impairment in adults over the age of 50. Macular degeneration can make it difficult or impossible to read or recognize faces, although enough peripheral vision remains to allow other activities of daily life.
The “dry” form of advanced AMD, results from atrophy of the retinal pigment epithelial layer below the retina, which causes vision loss due to the damage of photoreceptors, also known as rods and cones, in the central part of the eye.
The “wet” form of advanced AMD, causes vision loss due to abnormal blood vessel growth, ultimately leading to blood and protein leakage below the macula. Bleeding, leaking, and scarring from these blood vessels eventually cause irreversible damage to the photoreceptors and rapid vision loss if left untreated. Fortunately, only about 10% of patients suffering from macular degeneration have the “wet” type.
Macular degeneration is not painful, which may allow it to go unnoticed for some time. For this reason, regular eye examinations are important.
While approximately 10% of patients age 66 to 74 will have findings of macular degeneration, the prevalence increases to 30% in patients 75 to 85 years of age. Family history may also play a factor.
The good news is that regular eye exams, early detection and new treatment options, enable doctors to maintain and in some cases, increase visual acuity patients.
RETINAL TEARS AND DETACHMENTS
Retinal tears and detachments are conditions where the inner lining of the eye called the retina is damaged. The retina is a layer of tissue that’s light-sensitive and sends visual information through the optic nerve to the brain. If damaged, this layer of tissue can eventually detach from the inside of the eye, causing permanent vision loss.
A retinal tear describes a small break in this lining. Retinal tears can have many causes and can happen at any age. Retinal tears can be treated with laser surgery or an advanced “freezing” process. Both of these treatment options attempt to keep the retina in place and keep it from fully detaching.
Retinal detachment describes a much larger separation of the retina tissues and although it is not exclusive to older people, it’s more common in those over age 40. If detected with an eye exam early enough, retinal detachment can be treated with the procedures used for some tears, or with a more intricate surgery that uses gas to push the retina together with the wall of the eye to allow for reattachment.
Aging, eye trauma, eye surgery, or being drastically nearsighted may cause retinal tears or detachments. Symptoms of these retinal conditions may include seeing flashes or floaters, sudden blurry vision, and seeing an area of dark vision.
An eye exam is very important when these symptoms occur as permanent eyesight loss may occur if the retina problem is not treated in a timely manner.
Diabetic Eye Diseases
People with diabetes are at an increased risk of eye diseases like diabetic retinopathy and diabetic macular edema, which can lead to irreversible vision loss.
Diabetic retinopathy often progresses slowly and, like many eye diseases, may not present visible symptoms until irreversible vision loss occurs. Diabetic macular edema is quite serious and can impact the ability to read, write, drive, and recognize faces.
Both conditions can be identified early with a comprehensive diabetic eye exam. If you have diabetes, book your appointment now.
Glaucoma
Glaucoma is a problem when the optic nerve inside your eye is damaged from either having too high of a fluid pressure and or having many of the other risk factors involved.
This is called “the silent thief” as vision is lost slowly through destruction of the nerve fibers comprising the optic nerve, leading to side vision loss.
If not controlled, this can lead to eventual blindness.
We screen for glaucoma during our annual comprehensive eye examinations and if a suspicion arises, we will recommend that you return for further in depth glaucoma testing.
This testing will include extensive peripheral field analysis, 3D optic nerve digital photography, laser light imaging and measurements of the optic nerve as well as eye pressure profiles taken during different times of the day.
From these and other test results, we will determine whether you are presently diagnosed with glaucoma, a glaucoma suspect, or simply demonstrate glaucoma-like qualities but are completely normal for you.
Once the diagnosis is made, the doctor will explain your status and recommend the best course of action to fit the diagnosis.
There are several types of glaucoma. Click on each title to learn more.
Open-Angle Glaucoma
Fluid buildup caused by blockage of the eye’s drainage channels can increase intraocular pressure (IOP) and cause open-angle glaucoma. Generally, peripheral vision is the first thing impacted, followed by central vision.
Angle-Closure Glaucoma
Angle-closure glaucoma occurs when the space between the iris and cornea narrows, trapping fluid in the eye. When the pressure rises as a result of this fluid, angle-closure glaucoma occurs.
It can appear suddenly (acute) or progress gradually (chronic). Acute angle-closure glaucoma is a medical emergency. Sudden onset headaches, blurry vision, eye redness, or halos appearing around lights mean you should call your optometrist immediately.
Other Types of Glaucoma
Secondary glaucoma occurs when intraocular pressure is caused by eye trauma, injury, or infection.
When the optic nerve is damaged, but intraocular pressure remains within normal range, normal-tension glaucoma may be the cause.
Glaucoma Risk Factors
Glaucoma risk factors may include:
- A family history of glaucoma
- Extreme refractive errors
- Past eye injury or trauma
- Use of certain medications
- Heart disease, diabetes, or high blood pressure
Cataracts
As you age, the clear lens of your eye can thicken and become opaque. This is called a cataract. They are often the result of the normal aging process, though there are cases where cataracts are present at birth.
Symptoms of Cataracts
Cataracts generally develop without pain or redness. Some symptoms of cataracts might include:
- Foggy or blurry vision
- Difficulty seeing at night
- Seeing halos around lights
- Muted color vision
- Sensitivity to light
Preventing Cataracts
Cataract growth can be slowed by protecting the eyes from UV rays—a great pair of sunglasses can help! Eating foods rich in antioxidants like blueberries, apples, artichokes, and dark green veggies like kale and broccoli may also help to prevent cataracts.
Cataract Treatment
Often, obstructions to vision as a result of cataracts can be remedied through corrective lenses. But, cataracts can increase in size and may get to a point where glasses or contact lenses no longer provide the vision you want. In this case, we may recommend surgery.
If you’re having difficulty driving or performing your job safely, are struggling to watch television or read, or are experiencing challenges with daily activities that decrease your quality of life, it might be time to explore surgery.
Cataract surgery is safe and effective, and we will help you understand the procedure and your options.
Age-Related Macular Degeneration
Age-related macular degeneration (AMD) causes the breakdown of the macula, the area of the eye responsible for central vision. Damage to the macula can lead to central vision loss.
The central vision is responsible for reading, writing, driving, and recognizing faces, so any loss of vision in this area may make day-to-day tasks difficult.
People with AMD may not experience any pain or symptoms as the disease progresses. If straight lines begin to appear wavy or your central vision blurs in a way that glasses cannot correct, it’s time for an eye exam.
There are 2 types of AMD: dry and wet.
Dry AMD
Dry AMD is the most common type of AMD, accounting for the majority of cases. It occurs when parts of the macula become thinner due to aging and accumulate tiny clumps of protein.
Wet AMD
The less common type of the disease, wet AMD, is responsible for the majority of cases of blindness as a result of AMD. Wet AMD occurs when blood vessels grow under the retina and leak fluid into the macula.
We're on the Lookout for Early Signs of Eye Disease
Regular, comprehensive eye exams are the best defense against eye diseases that can cause irreversible vision loss.
Book your appointment today, and let us examine your eyes for early signs of eye disease so you can preserve sight of you and your loved ones.
Book AppointmentOur Brands